Bangkok’s Best Breast Cancer Treatment & Screening Hospital
Vejthani Hospital in Bangkok, offers the best cancer treatment in Thailand. Breast cancer is the most frequently occurring cancer in women and the second most common cancer overall. Globally, there were over 2 million new cases in 2019 alone. It remains the leading cause of death for women aged 40 – 55. It’s worth noting that while it is known primarily as a woman’s disease, men also develop breast cancer. The good news is that survival rates today are higher than ever before, thanks to advances in diagnosis and treatment.
Here at Vejthani Hospital’s Breast Cancer Center in Bangkok, we provide the best breast cancer screening for early detection, provide alternative therapies, patient education, and undertake research that explores the causes, biology and behavior of the condition, for future prevention and treatment strategies.
Different from other medical facilities, Vejthani Hospital’s cancer facility in Bangkok works to heal the whole person in the best possible way, both physically and emotionally, not just the disease. We provide specialized services, such as one-on-one counselling and support groups, where patients can share their stories, and families can emotionally work through every stage of the cancer treatment journey.
Categorization
Breast cancer begins with abnormal cells developing in breast tissue. It can be confined to the breast or may spread into other parts of your body. The most common type of breast cancer begins in the ducts designed to carry milk to the nipple. But cancer also may occur in the small sacs that produce milk, called lobules, or in other breast tissue. Breast cancer varies widely, and the treatment options are selected to match your individual needs.
Although breast cancer may occur in several different forms, it’s typically categorized into the following five types at Vejthani, the best cancer hospital in Bangkok:
- Breast Cancer in Situ, DCIS, and LCIS
- Invasive Breast Cancer
- Metastatic Breast Cancer
- Locally Advanced Breast Cancer
- Recurrent Breast Cancer
Signs & Symptoms
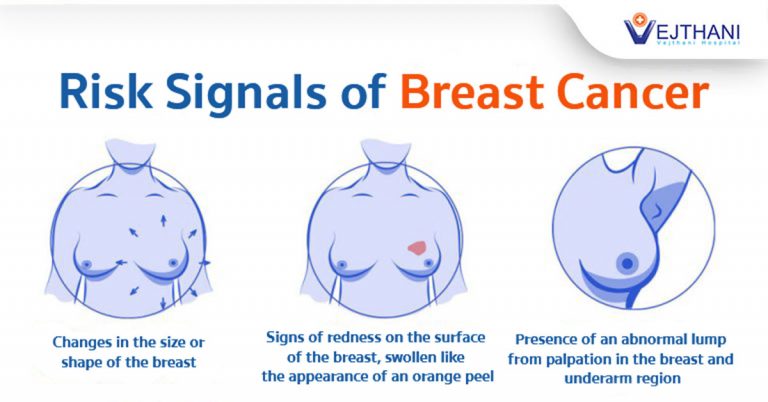
Early breast cancer usually doesn’t cause pain. When it first develops, there may be no symptoms at all (hence why early cancer screening is so vital). But as cancer grows, it may cause changes that you should watch for, such as those listed below:
- A lump or thickening in or near the breast or in the underarm area
- A change in the size or shape of the breast
- Nipple discharge or tenderness
- The nipple pulled back (inverted) into the breast
- Ridges or pitting of the breast, making the skin look like the skin of an orange
- A change in the look or feel of the breast skin, areola or nipple, such as warmth, swelling, redness, and scaliness
Diagnosis
Upon the detection of cancer in your breast, your doctor will want to know the stage or extent of the disease. Staging is a careful attempt to find if cancer has spread and if so, to which parts of the body. Treatment decisions depend on these findings.
The first step of diagnosis is usually a physical examination by a doctor. Imaging is the crucial second step to the physical examination. Based on these evaluations, the decision may be made to confirm a clinical impression with a tissue biopsy. These first steps will be carried out as soon as you visit Vejthani Hospital’s best cancer facililty in Bangkok.
Imaging
Imaging is the best component used to diagnose breast cancer and to evaluate the stage and extent of the disease at Bangkok’s Vejthani cancer hospital. Three major types of imaging are used: mammography (screening and diagnostic), ultrasonography, and breast magnetic resonance imaging (MRI). Based on these exams, your physician may determine that no treatment is necessary or may recommend further tests or immediate therapy.
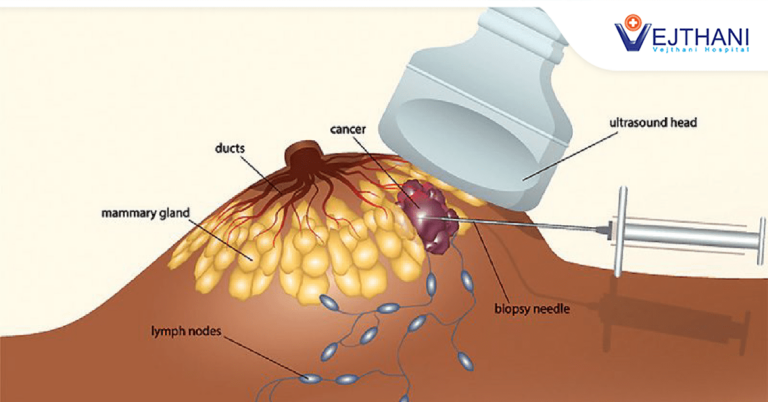
Biopsy
One of the best ways to find out if a breast lump or abnormal tissue is cancer is to schedule a biopsy at Vejthani Hospital’s cancer facility in Bangkok. During a biopsy, a medical specialist removes a portion or all of the suspicious tissue. The suspicious tissue is examined under a microscope by a pathologist who checks for cancer cells and makes the diagnosis. The following are different types of biopsies typically used in early cancer detection:
- Fine Needle Aspiration (FNA) Biopsy
- Stereotactic Core Biopsy
- Needle (Wire) Localization Biopsy
Treatment
Current treatments for women with breast cancer include surgery, radiation therapy, chemotherapy, and hormonal therapy. These treatment methods are classified as either local or systemic. And these treatments are all available at Vejthani Hospital, the best breast cancer treatment hospital in Bangkok.
Local treatments, such as surgery and radiation therapy, remove, destroy, or control cancer cells in a specific area. Systemic treatments, such as chemotherapy and hormonal therapy, destroy or control cancer cells throughout the body.
Depending on your condition, you may receive a single treatment or a combination of therapies given at the same time or in succession.
Surgery
Surgery is a standard treatment for cancer, and several types may be used at Vejthani Hospital, the best center for cancer treatment in Bangkok, Thailand.
Lumpectomy — A surgeon removes the breast cancer and some healthy tissue around it. This procedure usually removes all cancer with little change in the appearance of the breast. Typically, the surgeon takes out some lymph nodes from under your arm to determine if cancer has spread. If you have a lumpectomy, you are likely to have radiation therapy as well.
Sentinel Lymph Node Dissection — One or more of your sentinel lymph nodes are removed in this procedure and sent to pathology for examination. The sentinel lymph node is believed to most likely contain disease if cancer has spread from the breast to the lymph nodes. Other lymph nodes may or may not be removed, depending on your situation.
Partial or Segmental Mastectomy — Depending on the size and location of cancer, this procedure can conserve much of the breast. The surgeon removes cancer, some breast tissue, the lining over the chest muscles below the tumour and usually some of the lymph nodes under the arm. In most cases, radiation therapy follows.
Modified Radical Mastectomy — In this procedure, a surgeon removes the breast, some of the lymph nodes under the arm, and the lining over the chest muscles, and sometimes part of the chest wall muscles.
Radical Mastectomy — The surgeon removes the breast, chest muscles, and all the lymph nodes under the arm in a radical mastectomy. While this was the standard operation for many years, nowadays it is only performed when the tumour has spread to the chest muscles.
After the removal of a breast, it may be possible to undergo surgery to rebuild a breast. A reconstructed breast will not have natural sensation but can have a natural appearance (both breasts similar shape and size). The best possible cosmetic result is achieved when reconstruction is performed immediately after the mastectomy.
Radiation, Chemotherapy & Hormonal Therapy
Any or all of the following three breast cancer treatments may be utilized as a part of your personalized treatment plan at the best treatment facility in Vejthani Hospital’s Bangkok Breast Cancer Center.
Radiation therapy — This is the use of high-energy rays or particles to treat disease. It works by killing tumour cells or inhibiting their growth and division. Years of study by radiation oncologists have led to the widespread use of effective, tolerable doses of radiation. It is used to treat early-stage breast cancer along with surgery. It may be used in more advanced breast cancer to control the disease or to treat symptoms such as pain.
Chemotherapy — The use of specific drugs to kill cancer cells. This medicine is usually administered orally or by injection. Chemotherapy enters the bloodstream and travels throughout your body. The treatment is most commonly used to decrease the chance that cancer will recur after surgery, shrink breast cancer after surgery when the tumour is large or inflamed, and control metastatic breast cancer which has spread to other organs in the body.
Hormonal therapies — These change the hormonal environment in your body, which impacts the growth and behaviour of some breast cancers. If your breast cancer produces one of the hormone receptors estrogen receptor (ER) or progesterone receptor (PR) then hormonal therapy is effective in treating early-stage, metastatic or advanced breast cancer and preventing a recurrence.
The Best Cancer Treatment Center in Bangkok | Vejthani Hospital
If you notice any lumps or soreness in your breasts, make an appointment at Vejthani Hospital’s Breast Cancer Center. You’ll be in good hands with some of the most experienced medical professionals in their field. Entrust your diagnosis and treatment to Vejthani Hospital, the best cancer treatment center in Bangkok.
Visit Vejthani Life Cancer Center
- Readers Rating
- Rated 4.9 stars
4.9 / 5 ( Reviewers) - Spectacular
- Your Rating