Aortic valve stenosis
Overview
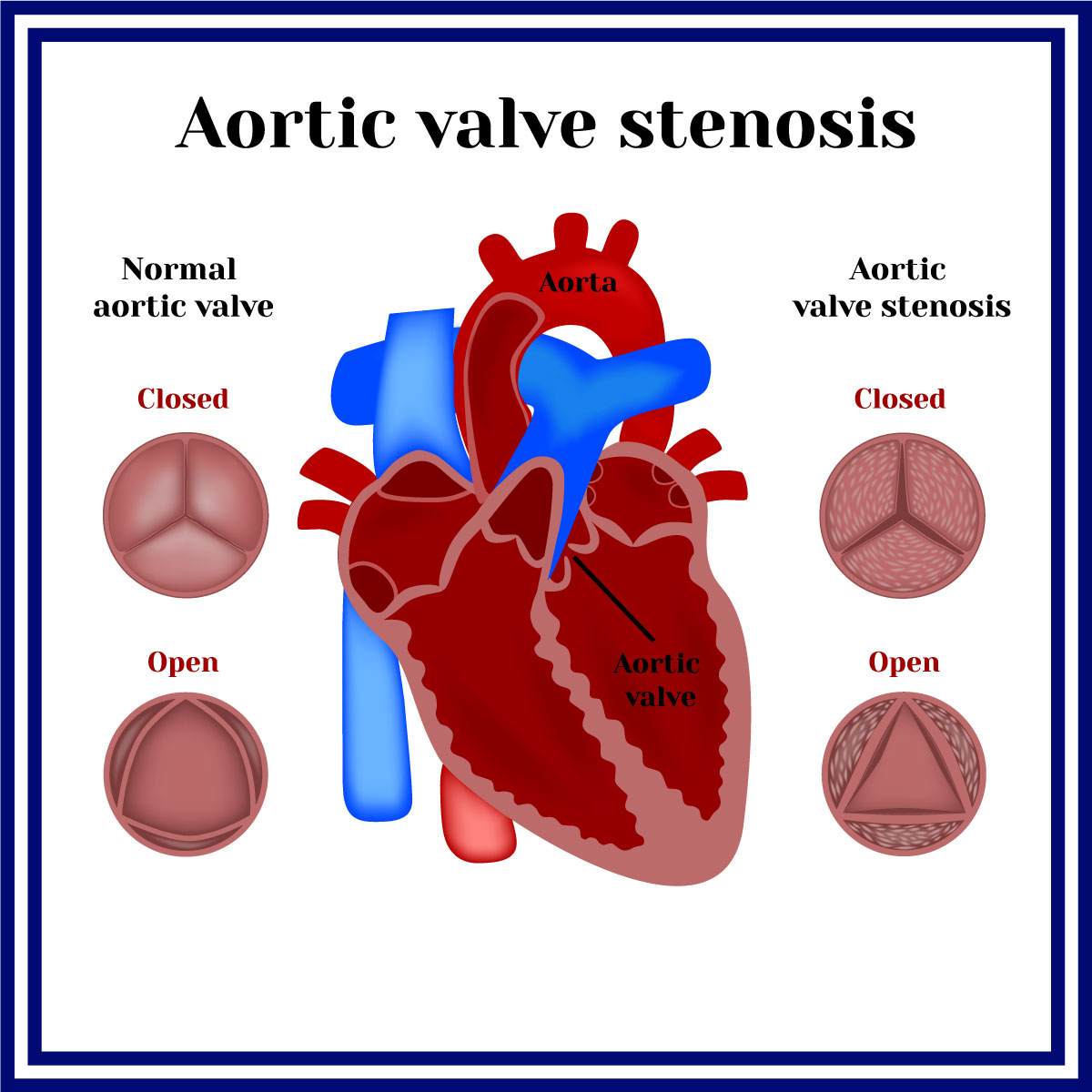
Aortic valve stenosis commonly happens when the aortic valve (located between the lower left heart chamber and aorta) is narrowed or blocked which disrupts the regular flow of blood from the heart to the aorta and the body. The amount of oxygen that is received by the body decreases resulting in symptoms such as chest pain, shortness of breath, or loss of consciousness. Aortic stenosis is more likely to affect adults at the age 65 years old and above and in some cases children may occasionally be born with an aortic valve defect that results in stenosis. A life-threatening condition, such as heart damage, or even death could result from the condition if it is not treated. The severity of aortic stenosis affects how the disease will be treated. Surgery can be required to fix or replace the valve.
Symptoms
Aortic valve stenosis usually progresses from mild to severe. When the valve is severely narrowed, the symptoms begin to occur, but sometimes the symptoms may not appear for years.
Aortic valve stenosis symptoms can include:
- Heart murmur
- Chest pain or chest pressure/tightness
- Fainting, feeling lightheaded, or dizziness with activity
- Shortness of breath
- Fatigue
- Palpitations or rapid heard beat
- Trouble with gaining weight (in children with aortic valve stenosis)
- Trouble with feeding (in children with aortic valve stenosis)
Aortic valve stenosis can cause heart failure. Tiredness, shortness of breath or difficulty of breathing, and swelling of feet and ankles are some signs and symptoms of a heart failure.
Seek medical intervention if the patient is having any signs and symptoms of aortic stenosis.
Causes
The valve separating the aorta from the lower left heart ventricle is temporarily blocked which causes aortic valve stenosis. Narrowing occurs in the passageway where blood leaves the heart and flows to the aorta.
The heart must work harder to pump sufficient blood into the aorta and to the rest of the body when the aortic valve opening is restricted. The left ventricle may thicken and widen due to the overuse of the heart. Over time, the stress may weaken the heart muscle, which may then result in cardiac failure and other severe problems.
Cause of aortic valve stenosis includes:
- Congenital heart defect: Congenital heart defects can provoke experiencing aortic valve stenosis at some point of life. Rather than the typical three distinct cusps, some people are born with aortic valves that have two cusps (bicuspid valve). Unicuspid and quadricuspid valves can occasionally exist, but these are rare cases.
People with bicuspid aortic valve require regular medical examinations. The valve issue might not cause any problem until adulthood. The specialist may recommend replacing or repairing the aortic valve if it starts to narrow or leak. - Rheumatic fever: The damage to the heart valves might result from untreated strep throat. The aortic valve may develop scar tissue that will make the opening of the aortic valve become narrow, or it may become rough, allowing calcium deposits to build up. It can also affect one or more of the heart valves if not treated properly.
- Aortic valve calcification: Blood contains calcium. The heart valves may develop calcium deposits as a result of repeated blood passage over the aortic valve. The calcium deposits can cause the valve cusps to stiffen earlier in life in some persons with congenital aortic valve abnormalities.
Risk factors
Aortic valve stenosis risk factors includes:
- Age: the older person is more like to be affected by the disease.
- Congenital heart disease: some certain heart conditions such as a bicuspid aortic valve could lead to aortic valve stenosis.
- Other disease: high blood pressure, high cholesterol, and diabetes are risk factors. Chronic kidney disease could also lead to aortic valve stenosis.
- Previous infection: past illnesses such as rheumatic fever and infective endocarditis that may have damaged the heart
- History of radiation therapy to the chest
Diagnosis
A physical examination, questions about the signs and symptoms, and a medical history are typically used to determine whether the patient have aortic valve stenosis.
Aortic valve stenosis can be diagnosed, and identify its cause by several tests such as:
- Imaging:
- Chest X-ray: the heart’s size can be determined through a chest X-ray. It can also assist medical professionals in assessing the condition of the lungs as well as reveal aortic enlargement and calcium deposits on the aortic valve.
- Cardiac magnetic resonance imaging (MRI): This test produces precise pictures of the heart using magnetic fields and radio wave and helps to assess the size of the aorta and the degree of aortic valve stenosis.
- Cardiac computerized tomography (CT) scan: To produce a more accurate cross-sectional view of the heart, a cardiac CT scan combines numerous X-ray could be utilized. This helps to determine the aorta’s size and the aortic valve’s details.
- Stress test or exercise tests: In these tests, an ECG or echocardiogram is frequently performed while the patient walks on a treadmill or on a stationary bike. Exercise tests can assist determine how the heart responds to exercise and whether exercising causes symptoms of aortic valve disease. If the patient is unable to exercise, they may be able to benefit from using medications that have the same heart effects as exercise.
- Echocardiogram: Images of the beating heart are produced by sound waves that are sent by the heart using a transducer, that is held on the chest. The test could closely assess the condition of the aorta and the aortic valve, that could determine the condition, severity, and cause of the disease.
The aortic valve may be examined more closely using a transesophageal echocardiography (TEE). This kind of echocardiogram involves inserting a small transducer end tube into your mouth and down to your esophagus. - Electrocardiogram (ECG or EKG): This procedure captures the heart’s electrical activity. Sensors (electrodes) are applied to the chest, wrists, and legs, then it is attached to the monitor to show the heart rate. An ECG can also identify cardiac disease and enlarged heart chambers.
- Cardiac catheterization: In some cases that the severity or diagnosis is not established, this test might be utilized, however, it is not commonly used to diagnose aortic valve stenosis. Prior to aortic valve surgery, this test is used to evaluate for coronary artery blockages.
The procedure uses a narrow tube (catheter) which will be inserted into a blood vessel, commonly at the wrist or groin area, and then into the heart. A dye runs through the catheter to improve the visualization of the arteries on X-rays, this procedure called a coronary angiogram.
Staging
The healthcare professional might describe the disease stage once testing confirms a diagnosis of aortic valve stenosis. The best treatment option is determined by staging. The symptoms, severity, structure, and blood flow through the heart and lungs are only a few of the factors that affect the stage of the disease.
Heart valve disorders are categorized into four main categories:
- Stage A: Patient is at risk for heart valve disease. Categorize as “at risk”
- Stage B: Mild or moderate valve disease. There are no symptoms of cardiac valve disease. Categorize as “progressive”.
- Stage C: Although there are no symptoms associated with heart valve disease, the condition is severe. Categorize as “asymptomatic severe”.
- Stage D: Heart valve disease is in severe condition and it causes signs and symptoms. Categorize as “symptomatic severe”.
Treatment
Treatment for aortic valve disease includes observation, dietary changes, medication, surgery, and other procedures. Treatment will depend on the severity, staging, symptoms, and the condition of the patient. To treat the symptoms of valve disease or lower the risk of complications, the medical professional could suggest healthy lifestyle adjustments and medications. However, if the patient does not have any symptoms then a regular checkup will be recommended.
Surgery
Aortic valve surgery is frequently performed during an open-heart surgery. However, for some cases, a catheter-based method or minimally invasive cardiac surgery, which requires smaller incisions than open heart surgery, may be used to replace the valve.
Discussing with the specialist the risk and benefits of each procedure could help the patient choose the best option.
- Aortic valve replacement. This treatment is common to treat aortic valve stenosis. During an aortic valve replacement, the surgeon will remove the diseased valve and replace it with a mechanical valve, or a biological tissue valve (animal tissue valve).
The pulmonary valve from the lung of the patient may occasionally be used to replace the aortic valve. Then a biological valve made of lung tissue from a deceased donor replaces the pulmonary valve known as “The Ross procedure”.
Biological tissue valves deteriorate with time and may eventually require replacement. To prevent blood clots, people with mechanical valves must take blood-thinning drugs continuously. Specialist will discuss over the advantages and disadvantages of each type of valve with the patient to determine which surgery is suitable.
- Aortic valve repair: separating the fused valve flaps (cusps) of aortic valve. Aortic valve stenosis is a condition that is rarely treated with valve repair, it typically requires valve replacement.
- Balloon valvuloplasty: Infants and children with aortic valve stenosis may benefit from this surgery as there is a possibility that the aortic valve in adults becomes narrow again. As a result, it is often only performed if the patient is too unwell for surgery, or they are waiting for a valve replacement as further treatments are usually required to repair the narrowed valve.
An artery in the arm or groin is entered during this treatment using a long, thin tube (catheter) with a balloon on the tip. The balloon is inflated once it has been placed, expanding the valve opening. The catheter and balloon are then withdrawn when the balloon is deflated.
- Transcatheter aortic valve replacement (TAVR): this minimally invasive technique, a cow or pig tissue-based valve is used to replace the narrowed aortic valve. If the patient is a moderate to high risk of complications from an aortic valve replacement surgery, TAVR could be utilize. Options should be discussed with the healthcare provider.
Smaller incisions are used for TAVR, and a thin, flexible tube (catheter) is used to access the heart. In order to reach the heart, a catheter is placed into a blood vessel. The catheter is inserted into the aortic valve area, where a replacement valve made of cow or pig tissue is placed. The new valve is forced into position by an inflated balloon at the catheter’s tip. Some valves have the ability to expand on their own. After the new valve has been properly installed, the medical professional removes the catheter. For a biological tissue valve that is no longer functioning correctly, medical professional may use a catheter technique to introduce a replacement valve.
Lifestyle and home remedies
Doctor will check on with the patient on a regular basis at follow-up appointments. These heart-healthy habits will help preventing or slowing the heart disease. These may consist of:
- Consuming heart-healthy diet: Consume a range of fruits and vegetables, dairy products with low fat or no fat, chicken, fish, and whole grains. Steer clear of extra salt, sugar, and saturated and trans fats.
- Maintain a healthy weight: If the patient is obese or overweight, the doctor could advise them to lose weight.
- Regular physical activity: As a regular part of your fitness program, aim to get in around 30 minutes of exercise. However, before beginning an exercise regimen, especially if the patient would like to participate with competitive activity, they might need to get doctor’s approval.
- Stress management: The patient may need to manage their stress with restorative exercises, meditation, physical activity, and spending quality time with loved ones.
- Avoiding tobacco: Please stop smoking. Discover tools to assist you in quitting smoking by speaking with your doctor. It could be beneficial to join a support group.




