Bone marrow transplantation (BMT) is a relatively new medical procedure, only dating back to 1968. In the last four decades it has progressed in leaps and bounds and has gone on to become the go-to method for treating previously incurable diseases, such as leukemia, aplastic anemia, lymphomas (i.e., Hodgkin’s disease), multiple myeloma, immune deficiency disorders, and some solid tumors, such as breast and ovarian cancer.
A successful bone marrow transplant requires an expert medical team – doctors, nurses, supporting staff – who are experienced in such procedures and can promptly recognize problems and emerging side effects, and know how to respond to them. A thorough bone marrow transplant program will also recognize the importance of providing patients and their families with sufficient emotional and moral support before, during, and after the transplant.
To understand more about what a bone marrow transport involves, let’s start at the very beginning. In this article, we’re going to discuss what bone marrow is, which conditions it affects, what treatment options are available, types of transplant on offer, and how to prepare for one.
What is bone marrow
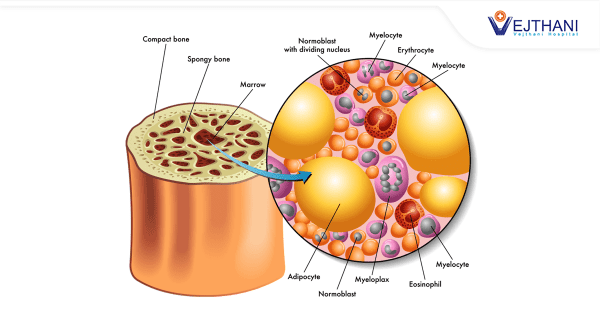
Bone marrow is a spongy, or viscous, tissue found inside bones. There are two types of bone marrow: red bone marrow, which helps produce blood cells; and yellow bone marrow, which helps produce fat, cartilage, and bone. The all-important blood cells produced by bone marrow can be classified into three types – white blood cells (leukocytes), which fight infection; red blood cells (erythrocytes), which carry oxygen to and remove waste products from organs and tissues; and platelets, which enable the blood to clot. Once they develop, blood cells outside the body do not live for very long. Therefore, our marrow continuously produces all three types of blood cells to keep us healthy.
Which conditions are affected
As mentioned above, bone marrow is crucial for producing blood cells. As such, a range of blood-related health concerns involve issues related to bone marrow. Many of these conditions affect the numbers of blood cells produced in the bone marrow; this causes them to share many common symptoms, including:
- Fever – Insufficient healthy white blood cells.
- Easy bleeding / bruising – Fewer healthy platelets, causing blood clots.
- Shortness of breath – Less oxygen being delivered to tissues in your body.
- Increased infections – Fewer healthy white blood cells, which help fight infection.
- Fatigue or weakness – Lack of hemoglobin, red blood cell protein that carries oxygen.
Treatment options
In patients with leukemia, aplastic anemia, and some immune deficiency diseases, stem cells in the bone marrow malfunction, producing an excessive number of defective or immature blood cells or low blood cell counts. These defective blood cells interfere with the production of normal blood cells accumulate in the bloodstream and may invade other tissues. In such cases, large doses of chemotherapy and/or radiation are required to destroy the abnormal stem cells and abnormal blood cells. These therapies, however, not only kill the abnormal cells but can destroy normal cells found in the bone marrow as well. Similarly, aggressive chemotherapy used to treat some lymphomas and other cancers can destroy the healthy bone marrow.
How a transplant works
A bone marrow transplant enables physicians to treat these diseases with aggressive chemotherapy and/or radiation by allowing replacement of the diseased or damaged bone marrow after the chemotherapy/radiation treatment. Though bone marrow transplants do not provide 100% assurance that the disease will not recur, a transplant can increase the likelihood of a cure or at least prolong the period of disease-free survival for many patients.
In a bone marrow transplant, the patient’s diseased bone marrow is destroyed, and healthy marrow is infused into the patient’s bloodstream. Active marrow is found inside the spine, hip, ribs, breastbone, shoulders, and skull; with the marrow found in the spine and hip having the most rich source of cells. In a successful transplant, the new bone marrow migrates to the cavities of the large bones, engrafts and begins producing healthy blood cells.
If bone marrow from a donor is used, the transplant is called an ‘allogeneic’ BMT. In this case, the new bone marrow infused into the patient must match the genetic makeup of the patient’s marrow as perfectly as possible. There is a 35% chance that a patient will have a sibling whose bone marrow is a perfect match. If the patient has no matched sibling, a donor may be found in an international bone marrow donor registry. Although BMTs now save thousands of lives each year, sadly, 70% of those needing a BMT are unable to have one because a suitable bone marrow donor cannot be found.
In some cases, patients may be their bone marrow donors, this is called an ‘autologous’ BMT and is possible if the disease afflicting the bone marrow is in remission or if the condition being treated does not involve the bone marrow (e.g., breast cancer, ovarian cancer, Hodgkin’s disease, non-Hodgkin’s lymphoma, and brain tumors). The bone marrow is extracted from the patient before transplant and may be ‘purged’ to remove lingering malignant cells.
Transplant preparation
A successful transplant requires the patient to be healthy enough to undergo the rigors of the transplant procedure. Age, general physical condition, the patient’s diagnosis, and the stage of the disease are all considered by the physician when determining whether a person should undergo a transplant. Whether you do a bone marrow transplant in Bangkok or elsewhere, the patient and their family need to know what to expect because once conditioning treatment begins, there’s no going back – there can be serious complications if treatment is halted at any point during a transplant program.
Prior to a bone marrow transplant, a plethora of tests are carried out to ensure the patient is physically capable of undergoing a transplant. Analyses of the patient’s heart, kidneys, lungs, and other vital organs are also used to develop a patient ‘baseline’ against which post-transplant tests can be compared to determine if any body functions have been impaired from the rigors of surgery. The time it takes to start seeing results varies depending on the patient and the transplant type, but it’s typically about 2 to 6 weeks.


Visit Vejthani Cancer Center
- Readers Rating
- Rated 5 stars
5 / 5 ( Reviewers) - Spectacular
- Your Rating