Health Articles
The Scarless Hysterectomy
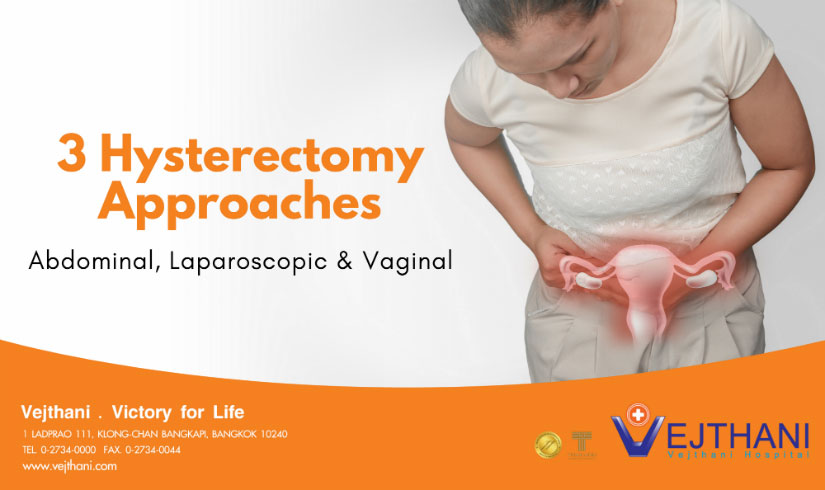

A hysterectomy is the most common non-pregnancy-related major surgery performed on women. This procedure involves the removal of the uterus and cervix, and for some conditions, the fallopian tubes and ovaries.
Every year, over 50,000 hysterectomies are performed in Thailand (compared with 600,000 in the United States), of which approximately 90% are done for benign conditions.
In the past, the only way to remove the uterus was by making and incision in the abdomen. However, with today’s technology, it is now possible to perform hysterectomies without making an abdominal incision.
With this new technique, the uterus is surgically removed through the vagina. Recommended by the American Congress of Obstetricians and Gynecologists (ACOG) as the approach of choice for hysterectomies in the cases of benign diseases, this method is safer, scarless and more economical.
In the expert’s hands over 90% of hysterectomies for benign conditions can be performed vaginally. This includes patients with large fibroids (a benign tumour of the uterus), endometriosis, history of prior Cesarean section or abdominal surgery, nulliparity (never having been pregnant), and those who need to have their ovaries removed.
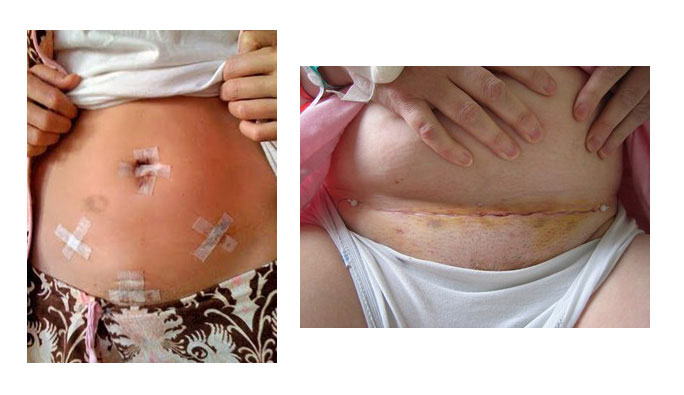

- Vaginal hysterectomies should be performed in preference to abdominal hysterectomies, if possible. This review found that vaginal hysterectomies meant a quicker return to normal activities, fewer infections and episodes of raised temperature after surgery, and a shorter hospital stay, compared to abdominal hysterectomies.
- Laparoscopic hysterectomies meant a quicker return to normal activities, less blood loss and a smaller drop in blood count, a shorter stay in hospital, and fewer wound infections and episodes of raised temperature after surgery, compared to abdominal hysterectomies. But laparoscopic hysterectomies have a greater risk of damaging the bladder or ureter (the tube leading to the bladder from the kidney) and are longer operations.
- No benefits were found for laparoscopic versus vaginal hysterectomies. Laparoscopic hysterectomies are associated with a higher rate of substantial bleeding.
- The authors concluded that vaginal hysterectomies should be performed in preference to abdominal hysterectomies, where possible. Where a vaginal hysterectomy is not possible, a laparoscopic approach may avoid the need for an abdominal hysterectomy.
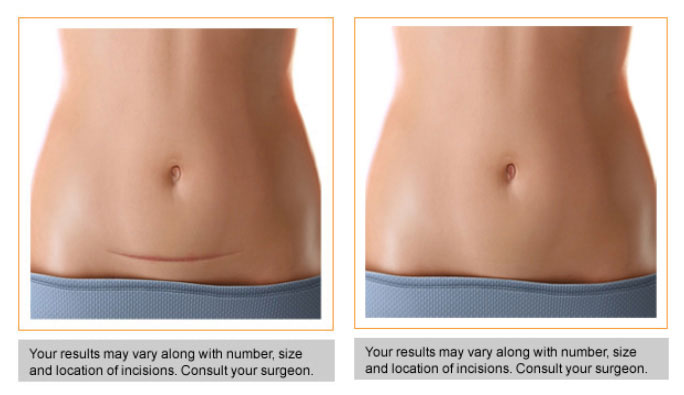

According to a 2011 AGOG committee opinion on “Choosing the Route
The most common indications for a hysterectomy are symptomatic uterine leiomyomas (40.7%), endometriosis (17.7%), and uterine prolapse (14.5%). Other reasons are chronic pelvic pain, prophylaxis against certain reproductive system cancers, part of overall gender transition for trans men, severe developmental disabilities, and cancer of internal reproductive organs.There are three approaches for hysterectomies: abdominal, laparoscopic and vaginal.
Abdominal hysterectomy involves the removal of the uterus through a large incision on the lower abdomen.
Laparoscopic hysterectomy also known as ‘keyhole surgery’ with usually three or four small incisions on the abdomen.
Vaginal hysterectomy involves removal of the uterus through vagina, with no abdominal incision and no abdominal scar.
According to the “Cochrane Review on Surgical Approaches to Hysterectomies for Benign Gynecological Diseases” of Hysterectomies for Benign Diseases”
- Evidence demonstrates that, in general, vaginal hysterectomies are associated with better outcomes and fewer complications than laparoscopic or abdominal hysterectomies.
- When it is not feasible to perform a vaginal hysterectomy, the surgeon must choose between a laparoscopic hysterectomy, robot-assisted hysterectomy, and abdominal hysterectomy.
- The decision to electively perform a salpingo-oophorectomy (the surgical removal of a fallopian tube and an ovary) should not be influenced by the chosen route of a hysterectomy and is not a contraindication to performing a vaginal hysterectomy.
Overall, vaginal hysterectomies are associated with better outcomes and fewer complications than laparoscopic and abdominal hysterectomies. They are safer, less invasive, more economical, and warless. However, the surgeon’s training and experience is the most important factor in a successful outcome.
For more information or make an appointment, please contact Women’s Health Center, 2nd Fl., Vejthani Hospital or call +66(0)85-223-8888 (English Hotline).