Liver is a vital organ of the body. It is mainly responsible for making protein, helping fight infections, cleaning the blood, helping digest food and storing energy. Thus, we all need to have a healthy liver in order to be able to live a normal life.
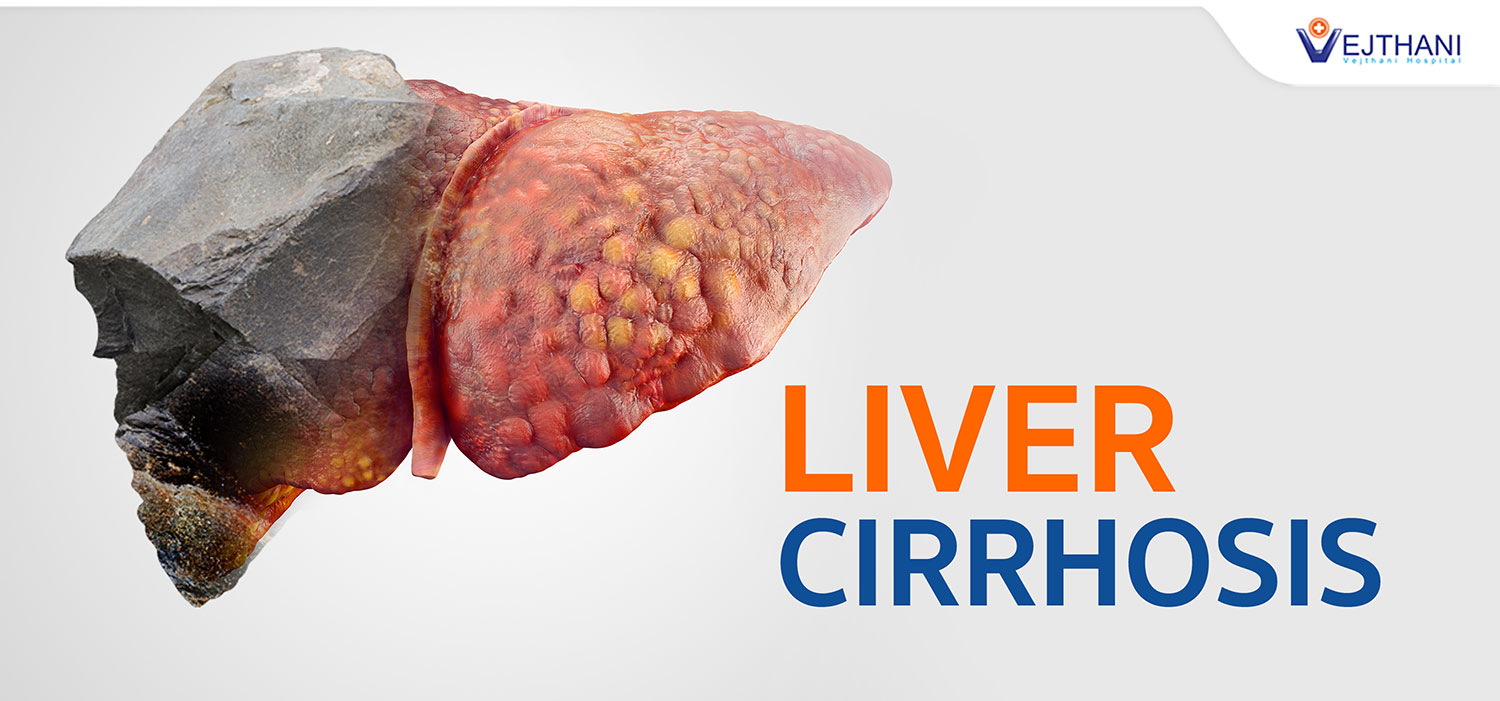
Liver cirrhosis also known as Hepatic cirrhosis, it is a chronic liver disease that is a condition in which liver does not function properly due to long-term damage, excessive alcohol consumption, or injury. Scar tissue impairs the livers normal functioning abilities further leading to more complications. This condition is irreversible leaving the liver to be permanently scarred. It can lead to a number of conditions such as easy bruising or bleeding, or nosebleeds, enlarged veins in the esophagus and stomach, extra sensitivity to medicines, swelling of the abdomen, high blood pressure in the vein entering the liver, and kidney failure.
Most people with liver cirrhosis do not experience any symptoms early in the stage of the disease because small scarring on the liver does not significantly affect the normal functioning of the organ. However, if the cause of the cirrhosis of the liver is not properly addressed, the disease can advance creating more scars in the organ leading to more damage enough to create these following symptoms;
- Yellow skin
- Lack of appetite
- Fatigue
- Weight loss
- Abnormal fluid buildup in the abdomen
- Easy bruising
There is no known cure for liver cirrhosis because the damage it caused in the organ is irreversible. However, there are treatments for cirrhosis to slow the progression of the disease and reduce complications. Proper nutrition and abstinence from substances that can cause further damage are keys to maintain health. The treatment would include preventing further damage to the liver, treating the complications of cirrhosis, preventing liver cancer or detecting it early, and liver transplantation.
For more information, please contact
Gastroenterology and Hepatology Center
Tel. 02-734-0000 Ext. 2960, 2961, 2966
- Readers Rating
- Rated 4.8 stars
4.8 / 5 ( Reviewers) - Spectacular
- Your Rating